The rebel scientists often find themselves at odds with the scientifically suspect logic behind the scheduling of certain drugs. The federal government’s five schedules under the Controlled Substances Act have a way to demonize those that they classify.
But with verifiable and reproducible data, which are ironically, yet necessarily, funded by the federal government, the scientist can make a sound case that some notorious drugs actually have redeeming qualities, and thus can help de-demonize narcotics that have been historically blacklisted.
Perhaps even the government itself is a silent rooter for the cause of such rebel scientists; the National Institute on Drug Abuse, or NIDA, approves 99 percent of requests, which floats at around 400 per year, from DEA-licensed researchers who are looking to study illegal or classified drugs. But, while the government is willing to fund essential research, the question remains whether it would be equally willing to start removing or demoting drugs based on new and thoroughly substantiated data. It seems only time will tell.
In the meantime, scientists are hard at work to find the good in scheduled drugs. Not including marijuana since its medicinal effects are already highly marketed, here are three others whose potential benefits are lesser known, but are nevertheless inspiring new medical treatments for certain disorders, particularly those that affect mental health.
1. Ketamine for Depression
Initially developed as a cleaner, or less psychosis-inducing, version of the anesthetic phencyclidine, ketamine has recently gained fame for its rapid antidepressant effects in both bipolar and, more notably, major depression.
The known schedule III anesthetic, which is also a horse tranquilizer and a chemical cousin to PCP (angel dust), was first clinically tested on depression when scientists used it as an NMDA receptor antagonist to test the role of NMDA receptors in depression. A 2000 double-blind study found that ketamine significantly improved depressive symptoms within 72 hours. But this study only included seven subjects.

When the pool size increased from seven to seventy-three, as in the well cited 2013 study, the conclusion fared even better for ketamine’s case against depression. In the study, chronically depressed individuals were randomly assigned to groups that either used ketamine or benzodiazepine midazolam, which is also an anesthetic but serves as the study’s placebo control since it doesn’t act as an NMDA antagonist.
The researchers remarkably found that, just after twenty-four hours, 74 percent of the ketamine group reported an alleviation of depressive symptoms, while only 28 percent of the midazolam group did. The results seem to show that ketamine works as an antidepressant because of its NMDA receptor-blocking properties.
But apparently, some other NMDA blocking properties don’t affect depression at all and current ketamine “copy cats,” though fairly effective antidepressants, are not nearly as potent as the parent drug. And since “Nature” published a 2016 study that concluded ketamine’s byproducts, not the drug itself, could be responsible for lowering depression via a non-NMDA network, new theories beyond the NMDA are rising above the horizon.
In fact, later this month, researchers will convene at a meeting for the Society of Biological Psychiatry to present findings that the hand behind ketamine’s antidepressant power might not even involve neurons, but rather glial cells, which are non-neuronal brain cells that support neurons. Regardless, the future of a ketamine-inspired medication is indeed very bright.
2. MDMA for Post-Traumatic Stress Disorder (PTSD)
The popular party drug MDMA (or ecstasy, though some claim that the two terms are somehow different) was created by a German chemist in 1912, fell off the map and later remerged in the 1970s.
Before the U.S. listed MDMA as a schedule I drug in 1985, a study suggested that MDMA was particularly useful in helping patients open up during their psychotherapy sessions. In fact, some even called it the “penicillin for the soul.”
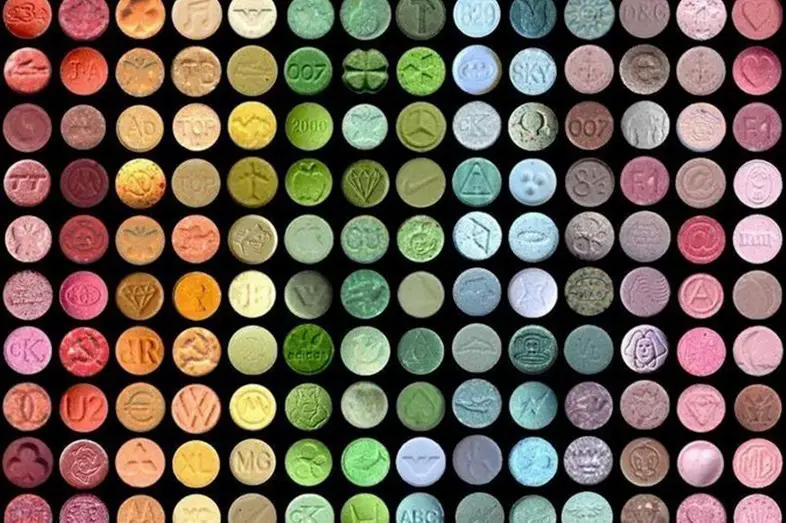
A couple of decades later, scientists caught wind of MDMA’s potential promise, and, in 2010, Mithoefer and colleagues performed the first randomized controlled pilot study of MDMA-assisted psychotherapy for PTSD. The 2010 study found that 83 percent of the MDMA group reported a marked decrease in PTSD symptoms, while only 25 percent of the placebo group did. After a few years, the same researchers followed up on their study, and found that 74 percent to 89 percent of those participants had long-term improvement.
So why does MDMA, in conjunction with therapy, work so well to treat PTSD? The current hypothesis is that it increases sociability, enhances therapeutic trust and gives the host more access to emotionally-upsetting material.
Interestingly, according to a 2012 study, healthy volunteers who were given MDMA found that friendly faces were easier to spot, while they found the hostile ones harder to identify. And by increasing levels in serum oxytocin, which is thought to play a large role in forming intimate bonds, MDMA helps patients to trust their therapists more during sessions, and thus increases the effectiveness of psychotherapy.
The promising results of MDMA in clinical trials are not being ignored; in fact, the now illegal drug is quite close to becoming an FDA approved medication. Most recently, at the Psychedelic Science 2017 conference, researchers presented unpublished data of MDMA from phase II trials, and the FDA recommended that the drug now move to phase III, which is the last step before potentially inheriting legal status.
Of course, the final phase will take the longest to process at about seven years, but then again MDMA, which has stayed under schedule I for the past 30 years, could now become legal within the next decade.
3. Magic Mushrooms for Depression and Anxiety
The prehistoric magic mushrooms contain psilocybin, which is an agonist for a specific serotonin receptor that SSRIs, a commonly prescribed anti-depressant, don’t directly target. But psilocybin, though unique in attack, seems to have anti-depressant properties just the same. A 2016 study found that participants with treatment-resistant depression noticed a sharp decline in their symptoms after both one week and three months since ingesting a high dose of the psychedelic.

But perhaps the most telling evidence of psilocybin’s powers is the drug’s effects on cancer patients who are depressed and anxious from their ill condition. In a study published late last year, Johns Hopkins researchers randomly assigned 56 subjects into one of two groups that administered either low-doses (as placebo control) or high-doses (for testing) of psilocybin.
They found that, after six months, 80 percent of the high-dose group felt that their end-of-life depression and anxiety were significantly reduced, with over 80 percent of the same group testifying that they generally enjoyed life more. Another study that was published on the same day as the Hopkins paper confirmed the incredible efficiency of the psychedelic in helping cancer victims feel less depressed and anxious about their fateful lives.
The results of psilocybin, which is a Schedule I drug, in fighting depression is profound enough that David Nutt, a director in the division of brain sciences at Imperial College London, said, “I’m absolutely sure that, within ten years, psilocybin will be an accepted treatment for depression.” If Nutt is right, then the legal versions of psilocybin and MDMA seem likely to end up on the public market at the same time.
These three drugs—ketamine, MDMA and magic mushrooms—are precisely regulated because of their negative side effects and potential for abuse. And though the government has good reasons for classifying drugs the way it does, many of those reasons were based on data that are now defunct and outdated.
And as the prime engine in the war against the unfair treatment of scheduled drugs, scientists are churning up more data that certain drugs, especially a few under schedule I, may deserve a looser federal treatment. Hopefully, the government will pay heed to the intense amount of research that counter the typical view towards scheduled drugs as completely heinous, and will perhaps keep an open mind to a possible reclassification of drugs based on new and upcoming data.

















[…] Study Breaks […]
Thank you for this insightful article! Your readers may be excited to know that they can directly contribute to the MDMA and psilocybin studies, as well as one on LSD microdosing, by participating in our crowdfunding campaign: http://www.fundamental.nyc
Our founder Rodrigo Niño spoke at the MAPS conference, and we just launched last week. Any support we can get will help us bring psychedelics that much closer to official, FDA-approved medicalization for treating mental health issues.
[…] Source: Beyond Marijuana […]
[…] initial plan and write the piece as if his story was the argument. I applied the same lesson to my Beyond Marijuana piece, which is laden with scientific data, by incorporating a sort of story, a theme, an […]
[…] be effective in treating depression and anxiety. Unlike other anti-depressants that run the risk of causing addiction, CBD has no addictive properties and no side effects. Instead, patients who use cannabidiol […]
[…] be effective in treating depression and anxiety. Unlike other anti-depressants that run the risk of causing addiction, CBD has no addictive properties and no side effects. Instead, patients who use cannabidiol […]