Sexually transmitted infections (STIs) are real, and they’re everywhere. Contrary to popular preconceptions, STIs are not rare misfortunes reserved for the promiscuous or the irresponsible; they are the unforgiving reality of many Americans — especially young ones.
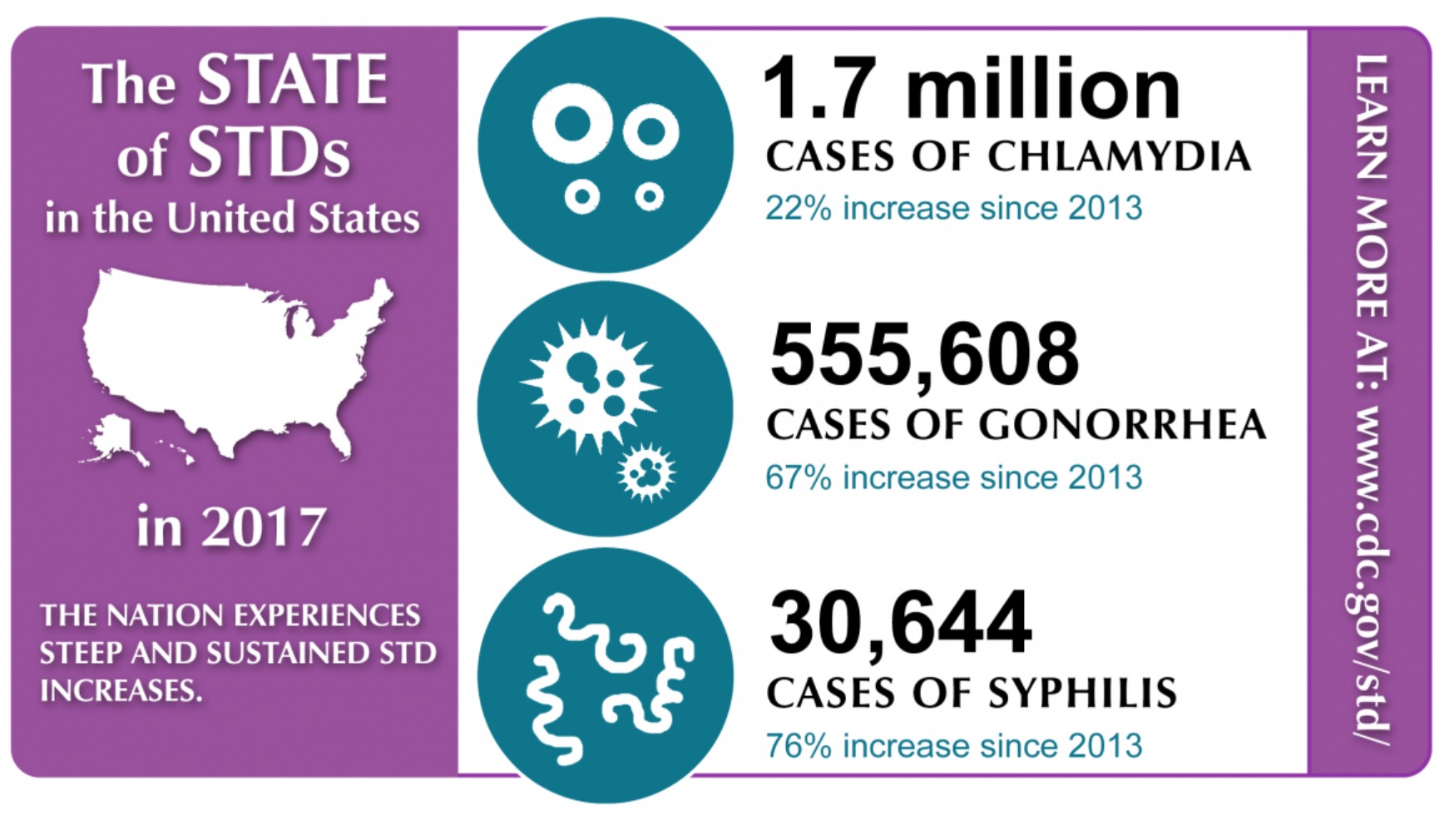
The Center for Diseases Control (CDC) approximated that over 20 million new STIs are diagnosed in the U.S. annually. Even worse is the fact that the CDC does not report STIs like human papillomavirus (HPV) or genital herpes, which would bring the count even higher.
The CDC’s 2017 report on the STI trends of that same year claimed to have reached a perturbing “record-high” that saw a disease like syphilis, which was almost entirely wiped out in past years, re-emerge with a vengeance and lead to more than 900 cases of congenital syphilis.
The hardest-hitting part about this crisis is the fact that many of the aforementioned infections are easily treated by a dose of antibiotics (whether the necessary medication is affordable is another issue altogether, albeit still a very pertinent one). However, the problem rests on the fact that many STIs, like chlamydia and gonorrhea, continuously go undiagnosed due to an absence of symptoms. The CDC reported that, if untreated, asymptomatic infections like chlamydia could result in long-term critical-health complications, such as infertility, chronic pain and susceptibility to HIV.
The tragic yet somewhat ironic nature of chlamydia points to the contradiction at the heart of the STI crisis today: the abundance and wide-scale availability of literature about the conditions and treatment of STIs, coupled with a growing public apathy about the reality of these infections.
In all fairness, there’s no denying that STIs are incredibly hard to openly talk about. In media and culture, they’re often characterized as the consequence of unmitigated sexual activity, with allusions to sexual impurity, lack of sexual cleanliness and promiscuity. Not to mention, they’re pretty embarrassing to bring up to friends and family, and seldom something you’d be more than happy to discuss with a sexual partner.
However, stigma is not the only deterrent to furthering a conversation about STIs. The circulation of misinformation regarding STIs and the regurgitation of urban myths are other factors responsible for this epidemic.
Take herpes, for example, a disease rampant with misinformation. Many people fail to realize there are two strains of the virus: herpes simplex virus-1 and herpes simplex virus-2 — the first one being “oral herpes” (the cold sore on the mouth) that 50 to 80 percent of Americans have, and the second being the STI.
Even genital herpes is not as fatalistic as media might like to paint it. While it’s true that there’s no known cure for herpes, people diagnosed with genital herpes can usually recognize the specific triggers that cause their outbreaks and effectively avoid them.
Reports by the American Sexual Health Organization also state that someone with the infection suffers from outbreaks as infrequently as once a year and that these outbreaks get progressively less severe. In this way, while blatant indifference to STIs is alarming, misguided paranoia can prove to be just as harmful, as it paints a distorted and inaccurate reality of what it means to live with an STI.
The less daunting reality is that while STIs are certainly unpleasant, most are far from a death sentence. Obviously, the severity of each individual infection is on a spectrum. There’s no question that an infection like HIV is significantly more serious than one like herpes (although it must be noted that even medication for something as malignant as HIV has made substantial progress in the last decades).
However, most STIs are curable, and those that don’t presently boast of a cure are still by all means manageable, given appropriate access to medication. This last piece of information is what you should cling on to if you find yourself terrified at the prospect of contracting one. At the end of the day, so long as you’re committed to the ongoing treatment of any present STIs and the prevention of future ones, you should take comfort in knowing that you’re doing everything in your immediate power.
The importance of practicing safe sex is another factor that cannot be emphasized nearly enough. While many people see condoms primarily as the means to prevent pregnancy, the use of condoms is essential to the prevention of STIs. Condoms — in contrast to other forms of contraceptives — are the method that most effectively prevents the spread of STIs by providing a barrier that significantly reduces the risk of transmission.
While the decision to engage in unprotected sex is ultimately a matter of personal choice, it undoubtedly comes with a variety of potential risks that could otherwise be reduced by the use of condoms. Although no one should be in a position to police you on your private sex life, it’s in your best interest to be fully aware of the stakes involved in having unprotected sex with a partner whose sexual health status you are not familiar with or cannot fully vouch for.
The truth is that a conversation on the crisis of STIs is long overdue. A case of this magnitude is reason enough for the issue to be elevated to the forefront of national sexual health campaigns and platforms. And while STIs shouldn’t inherently be something to agonize over, their pervasive nature — worsened by an insidious blend of ignorance and stigma that only fuels their proliferation — can no longer be overlooked.
So, let this be a public service announcement: Get in contact with your health care provider and schedule your next screening. Not only will you be taking an active role in the maintenance of your own health and well-being, but you’ll also be doing your part to break a larger chain of sexual disease.
Finally, while it’s crucial to tackle the deliberate disregard for the testing and treatment of STIs, it’s equally as important to reassure people that there is nothing shameful or demeaning about being diagnosed with one.